In this post
Introduction
Allergies are common in childhood, with 40% of children in the UK diagnosed with an allergy, especially hayfever, asthma, food allergies and eczema (Allergy UK). According to the Natasha Allergy Research Foundation (NARF), the most chronic childhood disorder is allergies, and 6-8% of children between 0-3 years old have a food allergy.
Some children may have relatively mild allergies, but others may have severe ones and are at risk of a severe allergic reaction if exposed to a specific allergen or allergens. While deaths from allergies are thankfully rare, they can be life-threatening. Therefore, it is vital to be aware of allergies in children and how they can be managed so they and their families can lead a happy and healthy life.
This blog post aims to provide information on common childhood allergies and how to recognise the symptoms. It will also give insights into allergy testing and some practical tips on managing and coping with allergies in children.
What Are Allergies?
Allergies result from the body’s immune system overreacting to a usually harmless substance, known as allergens or triggers, and some common ones can include:
- Certain foods, e.g. milk, eggs, peanuts, etc.
- House dust mites.
- Tree, weed and grass pollen.
- Pet dander.
- Mould.
- Insect stings, i.e. venom.
- Medications.
- Latex.
When an allergic individual first comes into contact with an allergen, their body perceives it as a threat, almost like a virus, and produces IgE antibodies. When exposed to the allergen again, their immune system mistakes it as harmful. An allergic reaction occurs when these antibodies recognise the allergen and release histamine, which causes allergy symptoms.
Some common allergens that can trigger allergic reactions in children are peanuts, cow’s milk, eggs, insect stings, pollen, house dust mites, and animals. Most allergies develop in childhood, but some will develop in their teenage or adult years.
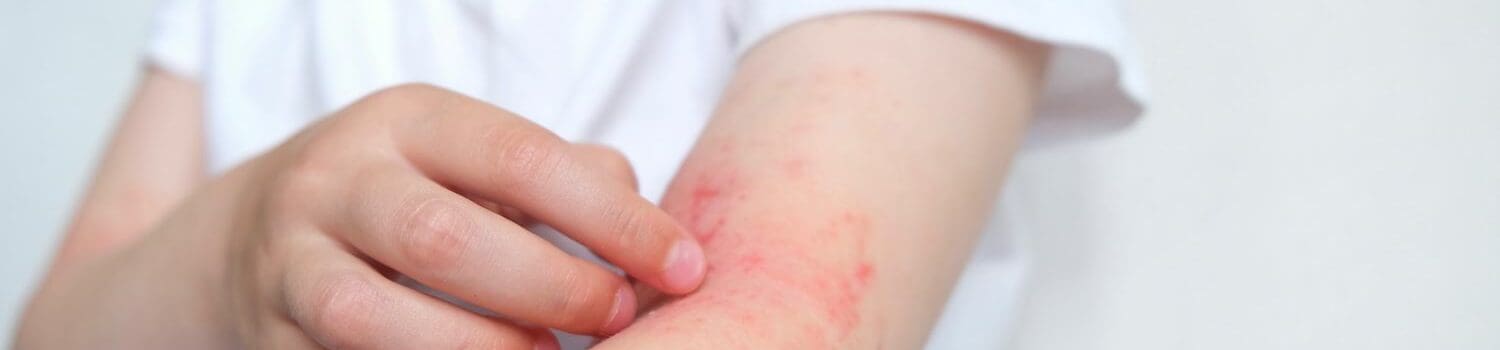
Types of Allergies in Children
There are numerous types of allergies, such as food, environmental, and insect stings.
Food allergies
There are 14 allergens recognised as being those that are more likely to cause allergic reactions, and these are:
- Celery.
- Cereals containing gluten (such as wheat, barley and oats).
- Crustaceans (such as prawns, crabs and lobsters).
- Eggs.
- Fish.
- Lupin.
- Milk.
- Molluscs (such as mussels and oysters).
- Mustard.
- Peanuts.
- Sesame.
- Soybeans.
- Sulphur dioxide and sulphites (if the sulphur dioxide and sulphites are at a concentration of more than ten parts per million)
- Tree nuts (such as almonds, hazelnuts, walnuts, brazil nuts, cashews, pecans, pistachios and macadamia nuts).
Children can be allergic to any of these allergens. However, they are more likely to be allergic to cow’s milk, peanuts, tree nuts, seeds, wheat, soya, shellfish, fish and eggs (BUPA). They have a higher risk of developing food allergies if they already have a food allergy, atopic eczema, asthma and hayfever or if there is a history of these conditions in the family.
Symptoms of food allergies can vary between children, but they tend to include the skin, respiratory system and digestive system. The latter symptoms, e.g. diarrhoea, vomiting, nausea and tummy pain, tend to be seen more in food allergies than other types.
Environmental allergies
Some allergens are environmental, meaning they are substances present in and around the environment in which we live. Children with allergic asthma and eczema are at a higher risk of developing these types of allergies. These allergies include hay fever, house dust mites, animals, etc.
Hayfever
Hay fever is an allergy caused by pollen released from trees, weeds and grass. It can impact sufferers throughout the year but usually during hay fever season, i.e. between late March and early September.
It typically develops in childhood or adolescence (NHS inform). According to Benadryl, 10-15% of children in the UK suffer from hay fever, and it is more common in boys than girls.
The symptoms of hay fever are similar to a cold, e.g. runny or blocked nose, sore throat, congestion and itchy/watery eyes. Children can also get earache, tiredness and headaches.
Dust mites
Dust mites are present in our homes, especially in carpets, bedding, clothing and soft furnishings. They are microscopic creatures that prefer humid environments and eat human shed skin.
Around one in twenty children will test positive for house dust mite allergy (North West Allergy Network). Children develop dust mite allergies because of the proteins in dust mite droppings, which are produced in large numbers daily. According to Allergy UK, they produce around 20 a day, and with millions of dust mites, that is a lot of droppings.
Symptoms of dust mite allergies in children tend to be similar to those seen in hayfever and typically affect the nose, eyes and respiratory system, e.g. runny or blocked nose, itchy, red or watering eyes and wheezing.
Animals
Children can be allergic to any animal, with allergies to cats and dogs being the most common. Children with pet allergies are allergic to a specific protein in the animal’s dander (shed skin), urine or saliva.
The symptoms of pet allergies usually affect the eyes and respiratory system, e.g. sneezing, runny or blocked nose, coughing, wheezing, watery, red and itchy eyes, nose rubbing, etc. In some cases, children may also get skin symptoms, e.g. rashes, hives or worsening eczema, especially if licked by a pet.
Environmental allergy symptoms
Allergies from environmental allergens tend to be known as allergic rhinitis, as symptoms tend to affect the nose after breathing in the allergen in the air. Unlike food allergies, environmental allergies do not tend to cause digestive symptoms, e.g. diarrhoea, stomach pain, vomiting and nausea.
Most children exposed to an environmental allergen tend to have mild reactions, unlike those with food and insect allergies, which can be more severe. However, if a child has asthma, environmental allergens can trigger asthma attacks, which can be serious and even fatal.
Insect sting allergies
There is no doubt that insect stings can be painful, especially for children. If a child is stung, they usually cry and have pain, minor swelling and redness around the sting site. However, this is not always a sign of an allergic reaction (Anaphylaxis UK).
When a child has an allergic reaction to an insect sting, it is because of the venom injected via a stinger into their skin. When they have a mild localised reaction, they typically have more swelling (i.e. greater than 10cm).
Some children may have severe allergic (systemic) reactions to insect venom, which can cause anaphylaxis. Symptoms of anaphylaxis will come on quickly, i.e. in minutes, and is a life-threatening medical emergency. These reactions can occur in anyone, especially if they have multiple stings or have been stung before.
Insects that sting include wasps, hornets, ants, solitary bees, honeybees, bumblebees, etc. It is important to note that bees and hornets rarely sting and will only usually do so if they feel threatened.

Recognising Allergy Symptoms
Allergy symptoms may differ depending on the type of allergen(s) a child is allergic to, their age and if they have any existing conditions, such as other allergies, atopic eczema and asthma. Here are some common allergy symptoms to look out for:
- Skin – redness, itchiness, rashes, hives (red welts).
- Respiratory – sneezing, runny or blocked nose, coughing, wheezing, breathlessness.
- Eyes – redness, itchiness, watering, sore.
- Digestive – tummy pain, nausea, vomiting, diarrhoea.
Symptoms usually start within a few minutes of being exposed to an allergen. However, in some cases, symptoms can develop gradually over a few hours.
It can sometimes be tricky to distinguish allergy symptoms from other childhood illnesses. For example:
- Allergic rhinitis symptoms from environmental allergens can be similar to the common cold or other viruses.
- A child with a common cold or other infections may have body aches, tiredness, a fever, a runny or blocked nose, congestion, sneezing and sore throat. With an allergy, they are also likely to have itchy, watery and red eyes and not a fever or body aches.
- A common cold will last for a few weeks, but if a child is exposed to an allergen, their symptoms are likely to persist, e.g. hay fever can last for months.
- Food allergy digestive symptoms can look the same as a stomach bug, i.e. gastroenteritis.
- Symptoms of gastroenteritis usually come on a day after infection and can include projectile vomiting, nausea and sudden/watery diarrhoea. Children will also typically have a mild fever, which is not usual in an allergy.
- Gastroenteritis symptoms usually last a week, but allergy symptoms will occur each time a child is exposed to a food allergen, typically straight after eating the food they are allergic to.
- Rashes and hives from allergies may get confused with other conditions, such as chicken pox, hand, foot and mouth disease, scarlet fever and even meningitis.
- There are numerous rashes, and the NHS has a useful guide with pictures.
- Allergy rashes and hives will typically occur with other allergy symptoms. Those caused by infections, e.g. bacterial or viral, are often accompanied by a fever, i.e. a high temperature.
To identify whether a child is suffering from an allergy rather than another illness, some of the following questions may help:
- What are their symptoms?
- Have they ever experienced these symptoms before?
- How quickly did the symptoms come on?
- How long are their symptoms lasting?
- Do they have existing conditions, such as asthma, eczema or any diagnosed allergies?
- Is there a history of allergies in the family?
- Do they have a high temperature?
- Have they been exposed to anything new, e.g. foods, animals and environments?
- Have they been around anyone with an infection, i.e. at nursery or school?
Parents and caregivers must always trust their instincts and contact their GP or NHS 111 if they have concerns.

Allergy Testing and Diagnosis
As allergy symptoms can mimic other illnesses and conditions, parents and caregivers need to seek advice from their GP if they suspect their child has an allergy. A GP will usually organise allergy tests or refer them to a specialist allergy clinic.
Allergy testing is important, as it ensures children receive accurate diagnoses to prevent allergic reactions, help manage their condition and improve their quality of life. It is critical for children with severe allergies, as exposure to an allergen can be life-threatening.
There are many ways of testing whether a child has an allergy, which can include:
- A skin prick or patch test – a small amount of the suspected allergen is put on the child’s skin to see if there is a reaction.
- Blood tests – a blood sample is taken from the child to measure the amount of IgE (allergy) antibodies in their blood.
- Special diets for suspected food allergies – a child avoids or eats less of a suspected food allergen to see if their symptoms improve.
Home allergy tests are available, e.g. test kits that give instant results and hair sample tests sent to laboratories. Healthcare professionals do not recommend them, as they can be unreliable, and only a blood test can identify an allergy. If a parent or caregiver suspects a child has an allergy, they should keep a diary of symptoms and see a GP.
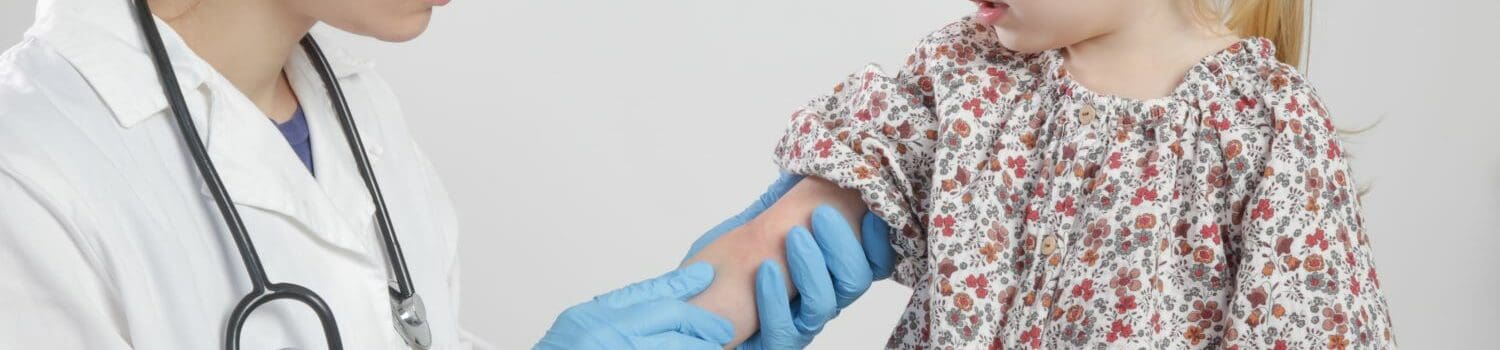
Managing Allergies
Once a child has been diagnosed with an allergy, it is important to manage their condition appropriately to reduce the risk of allergic reactions and lessen the impact on their and their family’s lives. It can be difficult for a child and their parents/caregivers, especially in the beginning or if their allergy is severe.
How to manage a child’s allergy will depend on the type and severity. GPs and specialist allergy clinics will typically provide advice and help on allergy management after diagnosis, but here are some practical tips and strategies that may also help:
- Avoid the allergen – it can often be tricky to avoid allergens, especially food and pollen, but there are ways to do this. For example, avoiding certain foods with allergenic ingredients, not getting close to stinging insects and staying indoors during high pollen days. Allergen barrier balms can also help to prevent airborne allergens from entering the body by trapping them.
- Administer medicines – antihistamines are the medicines commonly used to treat the symptoms of mild allergies. There are also steroid tablets/creams and nasal sprays. It is important to seek advice from a GP or pharmacist before administering any over-the-counter medicines.
- Have an allergy management and action plan – after a child has been diagnosed with an allergy, they will typically be given a personalised allergy management plan by their GP/clinic that details how to manage their allergy. If a child has a severe allergy, they are also likely to have an allergy action plan detailing the emergency actions to take if they have an allergic reaction.
- Carry emergency medicines – if a child has a severe allergy, they should carry at least two adrenaline auto-injectors (AAIs) with them at all times to be administered if they have a severe allergic reaction.
- Try immunotherapy – which is a desensitisation technique that involves exposing an allergic child to small amounts of an allergen over a specific period to allow their body to get used to it and reduce the severity of allergic reactions. It must only be conducted by healthcare professionals.

Food Allergies
One of the most common allergies in childhood is food allergies, which may be because their immune systems are still developing. According to the Natasha Allergy Research Foundation (NARF), more children than ever are being diagnosed with food allergies. Allergy UK estimates almost 1 in 12 young children suffer from a food allergy.
According to Allergy UK, children tend to be more susceptible to the following:
- Peanut allergy – affects around 2% (1 in 50) of children in the UK.
- Cow’s milk (protein) allergy – more common in babies and young children. Most will outgrow their milk allergy around five years old, but it can be lifelong in some. It is the most common cause of fatal food-induced allergic reactions in school-aged children (Imperial College London).
- Egg allergy – is more common in young children than in adults. However, most will outgrow it.
Tree nuts, cereals, soy, fish, shellfish and seeds can also be a problem in children. They are at a higher risk of developing a food allergy if they have eczema as infants, especially if it started early and was severe, or if they suffer from other allergies, such as hay fever and asthma.
To manage children’s allergies and reduce the risk of food allergic reactions, always:
- Check with GPs before cutting foods out of a child’s diet.
- Be aware of the food allergens a child is allergic to and understand the types of foods they can be in.
- Read food packaging and labels carefully before buying ingredients and giving children food. Manufacturers must emphasise any of the 14 allergens by law. These will be in bold, italics or underlined.
- Check menus carefully when eating out and ask staff if there is uncertainty about the allergens in their foods. Always inform them about the child’s allergies, as they may not guarantee food is allergen-free.
- Wipe down surfaces when eating out.
- Avoid foods if you are unsure whether they contain an allergen a child is allergic to.
- Inform family, friends, work, nursery and school about a child’s food allergy.
- Avoid cross-contamination when preparing and handling food, e.g. strict hygiene, thorough cleaning and disinfection and separate utensils. Certain foods may have to be banned from the home if a child has a severe food allergy.
- Keep an allergy kit close, which may contain an allergy action plan, antihistamines and AAIs.

Dealing with Allergic Reactions
How children, parents, caregivers and educators deal with allergic reactions will depend on their severity, the children’s ages and individual circumstances.
Mild/moderate allergic reactions
If a child has a mild/moderate allergic reaction, actions to take may include the following:
- Keep calm and reassure them.
- Check their symptoms to ensure it is an allergic reaction.
- Give them an age-appropriate antihistamine or prescription medicine where applicable.
- Have an inhaler nearby if they have asthma.
- Seek medical advice from a GP or NHS 111 if their symptoms are worsening/not improving.
- Seek urgent medical advice, e.g. calling 999 if symptoms are getting severe.
Severe allergic reaction
A severe allergic reaction can be a frightening experience for children, their parents/caregivers and nursery/school staff.
There is a risk of life-threatening anaphylaxis in children. According to Anaphylaxis UK, these serious symptoms are often called ABC symptoms, which are as follows:
- A – AIRWAY –throat, tongue or upper airway swelling (tightening of the throat, hoarse voice, difficulty swallowing).
- B – BREATHING – sudden onset wheezing, breathing difficulties (especially in asthmatics), noisy breathing, choking cough.
- C – CIRCULATION – dizziness, faintness, floppiness, sudden sleepiness, tiredness, confusion, pale/clammy skin, blue lips, loss of consciousness, unresponsiveness.
If a child has a severe allergic reaction, actions to take may include the following:
- Try to keep calm, as it will help you think more clearly.
- Use emergency medicines called adrenaline auto-injectors (AAIs) if they are available. Do not delay and use it, even if in doubt.
- Lie them flat and raise their legs, or sit them up with their legs raised if they are having difficulty breathing. Do not stand them up.
- Dial 999, ask for an ambulance and inform the operator that the child is experiencing anaphylaxis (severe allergic reaction).
- If their symptoms do not improve or worsen, administer a second AAI.
The step-by-step instructions for using an AAI will depend on the type, and there are three – EpiPen, Emerade and Jext. The instructions are on their websites, and the links are below.
If a child has an AAI, it is vital to ensure they carry two with them at all times. Also, check AAI expiry dates regularly to ensure they are in date.

Allergies and School
It can be difficult for parents and caregivers when their children are at school, as they will be away from the home environment. To reduce the risks to their children, it is vital to openly communicate with schools regarding their children’s allergies, as educators, support staff, and school nurses will have a role in managing them while they are at school. According to Anaphylaxis UK, at least one pupil has allergies in every school class.
If schools are unaware of children’s allergies and how to manage them, they will not know what actions to take to prevent allergic reactions or what to do if a child has an allergic reaction. Unfortunately, there have been cases where a lack of knowledge and awareness of allergies has led to child fatalities, with one tragic example.
Parents and caregivers must notify the school of their child’s allergy and provide them with a copy of their allergy management and action plans. They should also ensure they have any medication the child needs, such as AAIs. Schools should have allergy policies and procedures, and staff should have regular training. They have a legal duty to support pupils with medical conditions (Department for Education).
Schools should produce an individual healthcare plan (IHP) for children with allergies in collaboration with the child (where possible), parents, caregivers and an appropriate healthcare professional. They should also review it at least annually and keep it confidential. An IHP will typically include (this list is not exhaustive):
- The child’s name and address, date of birth and class.
- Details of their allergy and symptoms.
- Preventative measures.
- Their dietary requirements, medications and any other needs.
- Risks inside and outside of the classroom.
- The locations and accessibility of medications.
- Names of those responsible for administering medication.
- Any anticipated side effects from medications.
- Family contact information, e.g. names, addresses, telephone numbers and relationships to the child.
- The actions to take in an emergency, first aid and who to contact.
- Medical contact information, e.g. GP and hospital names, addresses and telephone numbers.
- Date of the plan and when it needs reviewing.
Children at risk of anaphylaxis must have an allergy action plan, which a GP or another healthcare professional should issue. Medical professionals must complete the plan and not parents or school staff. Schools must train their staff and follow the action plan if a child has an allergic reaction.
For further information see:
- BSACI – Paediatric Allergy Action Plans.
- Anaphylaxis UK – Allergy information for schools.
- UK – Allergy guidance for schools.
- UK – Supporting pupils with medical conditions at school.

Coping with Emotional and Social Aspects
It is not easy for children living with allergies or their parents and caregivers looking after them. It can be incredibly stressful and difficult to manage day-to-day, especially if their allergies are severe. According to Allergy UK, research has concluded that children with peanut allergies find it more stressful than those with long-term medical conditions, such as diabetes. Overall, allergies can have impacts on their mental health and well-being.
Allergies can also result in:
- Children feeling poorly, sleep-deprived and low because of their symptoms, which can lead to depression.
- Worry and anxiety about everyday activities and events, especially if a child has a severe allergy that could be life-threatening and has to carry medication with them everywhere.
- Social isolation, e.g. if a child cannot eat the same foods as other children at a Birthday party or if they cannot play outside when the pollen count is high. They may feel that they are different from other children.
- Lengthening the time to do simple tasks, such as shopping, cooking, laundry and cleaning, putting additional burdens on parents and caregivers.
- Children missing school because of their symptoms or the risks, which can affect their academic performance and future careers.
- Parents and caregivers finding it difficult to work because of the care and support their allergic child needs, which can impact the family financially.
There is no doubt that coping with allergies is difficult for children and their parents and caregivers. However, there are ways to cope, for example:
- Try not to feel anxious – it is hard for parents and caregivers not to feel anxious and stressed, but children can pick up on these emotions, which can also make them feel the same, potentially affecting them in adulthood. It is important to build confidence in children regardless of their allergies.
- Create a positive and supportive environment – parents and caregivers should openly communicate with their children and provide them with age-appropriate information and education regarding their allergies. Involving them as they get older is key.
- Plan meals – if a child has a food allergy, planning is essential, whether at home, school or eating out. For example, they could take their own food to a party. It is also vital to focus on the safe and tasty foods they can eat rather than solely looking at what they cannot eat.
- Do not restrict them unnecessarily – play and socialisation are vital for a child’s learning, development and overall well-being. Planning for any social occasion and openly communicating with anyone involved can help children to lead relatively normal lives.
- Get advice, help, support and guidance from charities – numerous charitable organisations can help allergic children and their families, e.g. Allergy UK, Anaphylaxis UK, BSACI, Sadie Bristow Foundation, the Natasha Allergy Research Foundation (NARF) and many others.
- Join support groups – plenty of groups online and face-to-face can provide support, e.g. Official Allergy UK Support Group and Sadie Bristow Foundation Allergy Support Groups.
Anaphylaxis UK has further information on ways to cope.
Conclusion
Allergies in children are common, especially food, hay fever, asthma and eczema, and can cause symptoms affecting their day-to-day lives, academic performance, socialisation and overall health and well-being. Allergies can also significantly impact parents and caregivers, especially if their children have severe allergies and are at risk of anaphylaxis.
While it can be difficult in some cases to identify whether a child has an allergy, it is vital to look out for the symptoms and seek medical advice if there are any suspicions. If a child is diagnosed with an allergy, it is understandable that they and their parents/caregivers will be worried and anxious about the future. However, understanding allergies and proper management can boost confidence, prevent allergic reactions, promote health and well-being and ensure a good quality of life.
If a child has a severe allergy, they must have appropriate allergy plans and emergency medications to reduce the risk of a severe allergic reaction and anaphylaxis. However, while it is sensible to be cautious, it is important not to “wrap them in cotton wool”. They need to live as normally as possible and play and socialise. Parents and caregivers should also remain calm, be confident and look after their own health and well-being.
There are plenty of resources, help and support for children and their parents/caregivers, so they should not feel alone. While it can be tricky to navigate, especially with severe allergies, it is possible through proper planning, education and good communication.



