In this post
Understanding the Term ‘Dementia’
Dementia is a term used to describe a group of symptoms which include loss of memory, the decline in the ability to think and reason, and issues with communication. There are a number of diseases and conditions that cause dementia, many of which will be described throughout this unit.
Dementia is thought to affect up to 850,000 people in the UK, with this figure set to rise to 1,000,000 by 2025. It is also estimated that by the age of 80, up to 1 in 6 people will experience some form of dementia. The cost of dementia to the NHS is believed to be in the region of £26 billion per year. Much research is continually being carried out to find a cure, because, at present, dementia is only manageable for a certain period of time.
According to the Diagnostic and Statistical Manual for Mental Health Disorders (DSM), the definition of dementia is: “multiple cognitive deficits, which include memory impairment and at least one of the following: aphasia, apraxia, agnosia or disturbance in executive functioning.”
A more accessible definition comes from the Cambridge English Dictionary, which defines dementia as: “a medical condition that affects especially old people, causing the memory and other mental abilities to gradually become worse, and leading to confused behaviour.”
The Most Common Types of Dementia
There are several types of dementia that are most commonly diagnosed; whilst each has some symptoms that are unique to the type, many will share symptoms, which can make diagnosing what type of dementia someone has quite difficult. The percentage of people who have each type of dementia within the UK are:
| Type of Dementia | % of Individuals Who Have This Type |
| Alzheimer’s Disease | 62% |
| Vascular Dementia | 17% |
| Mixed Dementia | 10% |
| Dementia with Lewy Bodies | 4% |
| Fronto-Temporal Dementia (Pick’s Disease) | 2% |
| Parkinson’s Dementia | 2% |
| Other Types of Dementia | 3% |
As might be expected, Alzheimer’s disease is by far the most common type of dementia amongst individuals within the UK. Mixed dementia happens when changes in the brain are caused by more than one type of dementia. The ‘other’ types of dementia, which 3% of the UK experience, are rarer forms of dementia, some of which include:
- Corticobasal degeneration (CBD)
- Creutzfeldt-Jakob disease (CJD)
- HIV-associated neurocognitive disorder (HAND)
- Huntington’s disease
- Multiple sclerosis (MS)
- Niemann-Pick disease type C
- Normal pressure hydrocephalus (NPH)
- Parkinson’s disease dementia (PDD)
- Posterior cortical atrophy (PCA)
- Progressive supranuclear palsy (PSP)
The Functions of the Brain That Are Affected by Dementia
The brain is the most complex organ in the human body and much of its capabilities are still not fully understood by researchers. It weights approximately 1.5kg and is the ‘control centre’ for everything that an individual does; including how they think, understand, remember and behave. It constantly adapts to the environment and controls how the world is experienced by the individual.
The brain is made up of billions of nerve cells that are connected to each other by something known as a ‘synapse’. The synapse enables messages to be sent between brain cells through chemicals and minute electrical currents. If brain cells die because of injury or disease, unlike most other cells in the body, they don’t regenerate and simply stop functioning, and this is what the fundamental cause of dementia is.
The brain is divided into four main parts:
- Cerebral hemispheres: This part of the brain consists of four separate ‘lobes’, all of which perform different functions
- Limbic system: The centre of the brain that is responsible for learning and memory
- Cerebellum: This part of the brain controls balance and movement
- Brain stem: This part of the brain controls automatic functions such as heart rate, blood pressure and breathing
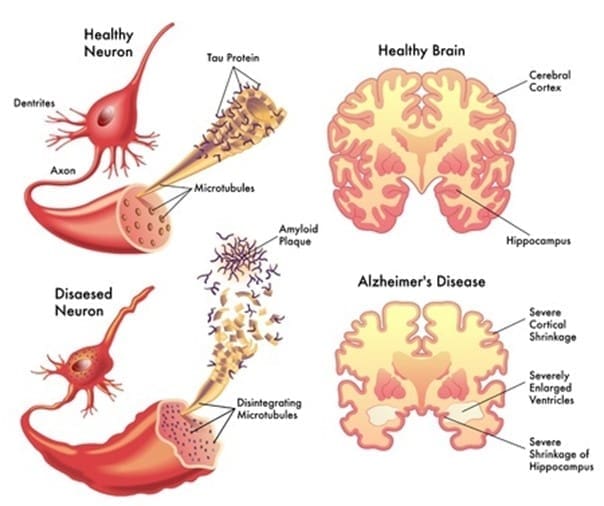
When someone has dementia, their brain physically changes because of the death of the brain cells, and the amount of change in the brain will depend upon what stage the dementia is at. During the middle stages of dementia, the brain’s cerebral cortex will begin to shrink and the brain vessels will become moderately enlarged. By the time dementia has progressed to severe, the brain ventricles will be extremely enlarged and the cerebral cortex will have shrunk even further.
The diagram below shows the deterioration of the brain in the case of an individual with Alzheimer’s disease – the right-hand side shows a brain prior to an individual having dementia to the later, more severe stages:
Cerebral Hemispheres
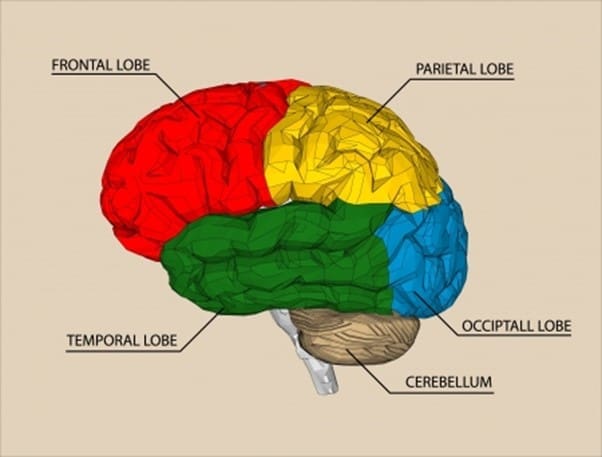
The cerebral hemispheres make up most of an individual’s brain; they are the main areas that are affected by the diseases and conditions that cause dementia. The cerebral hemispheres are divided into four lobes:
- Frontal
- Temporal
- Parietal
- Occipital
Whilst these four lobes have different functions, they all work together in order for someone to be able to carry out various tasks.
Frontal
The frontal lobe is responsible for an individual’s behaviour. Therefore, when cells in this area of the brain die out, then there will be noticeable changes in the way that the individual behaves. For example, someone who was previously very timid and shy might suddenly become loud and obnoxious; or someone whose character was laid back and relaxed may suddenly become anxious about everything. Damage to the frontal area of the brain may be very distressing for family members to witness. This is because it is common for individuals who have moderate and severe dementia to lose inhibitions, which can lead to aggression or to them losing sight of what is normal, socially acceptable behaviour. They may start to insult people, swear at them and even become violent. They may display behaviours which are completely out of context such as laughing when someone is crying or at a sombre occasion like a funeral.
Behaviour caused by frontal lobe changes can be extremely challenging and upsetting for family members and carers because when an individual’s behaviour changes beyond recognition, the person they used to be seems to have been ‘lost’ completely.
The frontal lobe is also responsible for movement, so when this area is damaged, it can affect an individual’s ability to walk and carry out other basic movement functions. When damaged, this lobe also inhibits a person’s ability to carry out movements that require smaller muscles, such as smiling or frowning. Because of this effect, it can often be difficult for individuals who have dementia to make themselves understood – much of communication occurs through body language, and when this is lacking, interactions can become difficult.
Another important function of the frontal lobe is enabling the individual to plan, organise and learn new tasks. It is common for people who have dementia to lose their ability to plan into the future because the skills needed to do this have been lost due to frontal lobe damage. Something as simple as making a cup of tea can become difficult because although this is a task that most people will take for granted, it still involves planning; putting the kettle on, getting the cups out, knowing when the water is ready etc. The frontal lobes also play an important part in working memory, which is the type of memory that involves holding information for a short time before either forgetting it or sending it to long-term memory stores. For example, repeating a phone number over and over so as not to forget it, is a function of the working memory. For someone who has dementia, this ability may be partially or fully lost, which can make carrying out the simplest of activities very difficult and frustrating.
Temporal
The temporal lobes are responsible for memory and language. The temporal lobes contain a part of the brain known as the hippocampus, which is thought to play a very large part in the storing and retrieving of memories. Therefore, damage to this area of the brain is what produces one of the most common symptoms of dementia: memory loss. Individuals who have memory loss can often not only have their ability to recall events affected but also their ability to remember names, objects and the sounds and smells around them and what they are associated with, which can be dangerous. For example, if someone who did not have dementia were to smell smoke in their home, they would immediately go and investigate where it was coming from in case there was a fire. Someone with dementia may not be able to make that link because they cannot remember that the smell of smoke is linked to fire and therefore to danger.
Damage to the temporal lobe inhibits an individual from taking part in a conversation, because individuals cannot recall the context of what something is or who someone is, so they cannot follow what is being said. Often they will struggle to process information fast enough to keep up and this can lead to frustrated and agitated behaviour.
Emotions are also regulated within the temporal lobes, and so when they are damaged, individuals may find that they can no longer regulate their emotions. They may become very angry or very sad but with no reason as to why this is happening. Very sudden changes in emotion can make daily living very difficult for the individual and for those around them as well.
Parietal
The parietal lobes handle information that is more complex, such as that which concerns size, space and perception as well as the ability to perform calculations and to spell words. Someone whose parietal lobes are damaged may find that they can no longer read words because they cannot make sense of the letters, as they become meaningless. Similarly, someone who used to be able to work out additions and subtractions in their head, will no longer be able to perform this task because of the damage caused in this area of their brain.
Movements such as eating and using a knife and fork are also compromised because this type of movement involves knowing about space – i.e. how far away the plate is and how far the hand must move in order to get there. Putting on clothes is something that most people can do without problems but this also involves the parietal lobes because people must know how far out to put their arm to put it into a sleeve and how far down they need to bend to reach their shoes.
Occipital
The occipital lobe controls vision, so any damage to this lobe will cause sight to be affected. On rare occasions, damage to the occipital lobe can be so severe that an individual will become blind.
Possible Causes of Dementia
Like so many other mental illnesses, the causes of most types of dementia have not yet been fully established. There are some factors which are known to contribute but they are not fully understood. The most that is understood is about the four most common types of dementia, which are:
- Alzheimer’s disease
- Vascular dementia
- Dementia with Lewy bodies
- Fronto-temporal dementia
Alzheimer’s Disease
Alzheimer’s disease is the most common type of dementia and accounts for up to two thirds of people who are diagnosed with the condition; it is named after Alois Alzheimer who was the first person to describe what the disease was.
Alzheimer’s disease is a progressive condition, which means that the symptoms will worsen as time passes, making people less able to maintain their independence and they therefore become far more reliant on other people.
During the course of the disease, proteins build up in the individual’s brain, which leads to structures that are referred to as a ‘plaque’ or a ‘tangle’ being formed. These structures that ‘block’ access to the brain’s cells mean that those cells are not given a sufficient supply of oxygen and nutrients, and because of this they will decay and eventually die. When this happens, dementia will occur because the area in which the brain cells have died will not be able to function.
It has also been found that individuals who have Alzheimer’s disease have a deficiency in the level of important chemicals in their brain that help to transmit signals. A shortage in the chemicals mean that these signals are not transmitted properly and therefore messages from the brain are not acted upon. For example, if someone wanted to tell another person about an event that they took part in the day before, they would have to retrieve that memory from a specific part of their brain (the hippocampus). If brain cells in that area do not have enough of the relevant chemical to send a message to the hippocampus to retrieve the memory, this will result in the individual simply ‘forgetting’ what happened.
There are certain risk factors that can also lead to Alzheimer’s disease, and whilst these might not be a direct cause, they may be a factor in its development:
- Age – people over 65 are at increased risk, with the chances of getting the disease doubling every five years after this age
- Gender – there are twice as many women as men over the age of 65 who have Alzheimer’s disease. The reasons for this are not currently understood
- Genetic inheritance – genetics are thought to play a small part in the onset of the disease, with people over 65 having more of a chance of developing it if one or both of their parents were affected
- Health and lifestyle – conditions such as diabetes, heart conditions and high blood pressure are thought to contribute to the onset of Alzheimer’s disease; although again, the reasons behind this are not fully understood
Vascular Dementia
This type of dementia is the second most common type after Alzheimer’s disease. Here, the word ‘vascular’ refers to the blood vessels that carry oxygen and other nutrients to all parts of the body – this includes the brain. When blood vessels do not receive what they need in order to continue functioning adequately, they will become diseased or will die, and this is what causes the symptoms of this type of dementia.
Certain conditions can cause levels of damage to the vascular system, and having one of them significantly increases the risk of developing vascular dementia. These conditions include high cholesterol, heart disease and diabetes.
Also, the incidence of a stroke can also cause damage to the vascular system, either in one major stroke or in a series of ‘mini strokes’ over time. Not everyone who has a stroke will develop vascular dementia but 20% of people who have a major stroke will develop it within six months after a stroke has taken place.
Someone who is affected by vascular dementia will see significant changes in their attention, memory and ability to use language effectively. The risk factors for developing vascular dementia are thought to be the same as those for Alzheimer’s disease.
Dementia with Lewy Bodies (DLB)
This type of dementia has similarities to Alzheimer’s disease because it too is thought to be caused by protein deposits (Lewy bodies) in the brain that affect the way in which messages between brain cells are sent. It also shares symptoms with Parkinson’s disease, and for this reason is often misdiagnosed. It is believed that DLB may actually be as common as occurring in 10–15% of all cases of dementia, but due to misdiagnosis official figures state that it only accounts for 4% of cases.
People who have DLB will likely be most affected by a change in their movements and cognitive abilities, often at the same time. There are no specific risk factors for DLB, other than age, with people over 65 being more likely to develop the condition.
Fronto-temporal Dementia
As the name suggests, this type of dementia affects the frontal or temporal areas of the brain; it is also known as Pick’s disease or frontal lobe dementia. Fronto-temporal dementia is caused by the death or disease of brain cells in the frontal or temporal lobes (located behind the forehead). It is also thought that a lack of relevant chemicals in this area in the brain also causes the cells to lose their ability to send messages to each other. As the disease progresses the lobes will actually physically shrink, causing the brain to appear quite different to before the condition took hold.
When this area of the brain is affected, individuals will see changes in their behaviour and their ability to recognise faces and familiar objects. It will also cause the individual to have problems with language.
There are no specific risk factors for fronto-temporal dementia but, for reasons that are not yet explained, it does seem more common in younger people, often being diagnosed between the ages of 45-65.
Other Causes
There are other conditions that are linked to the causes of dementia; these include:
- HIV/AIDS – in the later stages of HIV and AIDS, individuals are more prone to developing dementia
- Creutzfeldt-Jakob disease – although this is rare in humans it is a condition that is linked to dementia because it attacks the nervous system and gets into the brain where it destroys cells
- Korsakoff’s syndrome – this disease is linked to alcoholism and causes short-term memory loss. Although it is not considered to be an actual type of dementia, its symptoms are very similar to those of other types
The Likely Signs and Symptoms of the Most Common Causes of Dementia
Dementia is a progressive disease and, as such, its symptoms change as time passes. The Alzheimer’s Association have published a list of common ‘warning signs’ of any type of dementia, which is what individuals and their families should look out for before any formal diagnosis has taken place. The ten warning signs are:
- Short-term memory loss
- Difficulty planning ahead
- Forgetting how to carry out routine tasks
- Forgetting the time
- Difficulty with reading or with seeing objects
- Social withdrawal
- Poor judgement
- Consistently losing things
- Problems with coherent speech
- Sudden changes in personality
This stage is sometimes referred to as pre-dementia and is often mistaken for what would be normal aspects of ageing, which is why many individuals will ignore signs and symptoms because they simply believe that they are ‘getting old’.
Once a formal diagnosis of dementia has been made, the individual will be assessed to ascertain which stage they are at, and the outcome of this may depend on how long they have ignored the signs or how quickly the symptoms have worsened:
- Stage one – mild
- Stage two – moderate
- Stage three – severe
Stage One
At this stage, those who have dementia may be struggling to come to terms with any changes that they have noticed about themselves. They may try and hide signs and symptoms from loved ones because they are embarrassed, afraid or in denial about the changes that are happening to them – this can lead to social isolation, which is in itself a risk factor for other types of mental illness such as anxiety, stress and depression.
During the first (mild) stage, individuals may refuse to make any changes to their lifestyle but those closest to them are likely to notice subtle changes in their behaviours.
The most common signs and symptoms at stage one are:
- Memory lapses; problems in retaining new information and recalling recent incidents
- Changes in mood with frequent bouts of frustration or irritability, which can come on very quickly and without warning
- Have problems making decisions
- Losing track of what is being said in a conversation
- Changes in eating habits – individuals with fronto-temporal dementia are especially prone to this
- Have problems judging distance, resulting in clumsiness
- Loss of interest in hobbies and other activities that were previously enjoyable
- Consistently losing items around the house, such as keys or glasses
- Forgetting names and the word for common items, with the individual having to describe what they mean instead
- Getting lost or disorientated on journeys that were previously familiar
- Following instructions – this is very common in the onset of vascular dementia
- Visual and auditory hallucinations – only prevalent in those individuals with dementia with Lewy bodies, which can prove extremely distressing
Stage Two
By this stage, there has usually been a dramatic decline in memory and individuals will no longer be able to hide their symptoms from other people as they will be more reliant on care and support. By this point, someone may be acting as an unofficial carer or the individual may have chosen to receive some sort of formal care in their home. It is usually at this stage where friends and family who may have been in denial about their loved one’s condition are forced to face the truth because the individual may have undergone drastic changes in their personality and behaviour.
The most common signs and symptoms at stage two are:
- Severe lapses in memory
- Confusion about the time period that they are living in, which can lead to them believing that they are still responsible for childcare or that they have to go to work
- Mistaking family members for other people; for example, believing that their grandchild is their own son or daughter
- Reading and writing abilities have been drastically reduced or have even been fully lost
- For those suffering hallucinations, these will be worse and likely even more frightening
- Paranoia, with many individuals believing that family members are stealing from them, something which causes great distress amongst family members
- Many problems with social norms; for example, trying to get undressed in the street or swearing inappropriately
- There will be little or no understanding of written communication
- Sleep disorders occur mainly with those individuals who have DLB
- ‘Sun downing’ also occurs and is where the individual’s symptoms seem to worsen as the daylight fades, which can often lead to wandering in the middle of the night
Stage Three
By this severe and advanced stage, the individual will almost certainly be wholly reliant on caregivers. Those caregivers may be finding the individual to be too difficult to manage and so this stage is when individuals are most likely to transfer to living in residential accommodation. They may be more likely to exhibit behaviour that challenges others, becoming increasingly aggressive or socially inappropriate.
The most common signs and symptoms at stage three are:
- Speech has often been reduced to simple sentences or sometimes even a single word or a cry
- Incontinence
- An inability to feed themselves will be common for an individual who may not even realise when it is time for them to eat a meal
- Apathy, where the individual will simply sit for hours at a time without any movement or interest in anything else
- No personal hygiene routine; individuals may not be able to remember how to care for themselves because many activities involved are required to be completed in a specific order, which the individual cannot replicate
- Muscle mass usually deteriorates causing individuals to spend a lot of time in bed
Despite all of the common symptoms across different types of dementia, it is crucial that families and caregivers remember that everyone will experience dementia in a different way. Being alert to changes as the disease progresses will help both individuals and their families to cope better at what can be an extremely difficult time for many people.
The Difficulties Individuals with Dementia May Face in Day-To-Day Living
Memory consists of two main storage areas; these are short term and long term.
Short-term memory refers to the aspect of memory which acts in the same way as a notepad – it enables individuals to hold information for a short space of time (up to approximately 30 seconds) so that it can be recalled immediately for usage or it can be sent to be stored in long-term memory where it can be recalled if required in the future. An example of short-term memory is when someone is reading a sentence – the start of it needs to be held in the short-term memory in order for the rest of it to be given context, otherwise it wouldn’t make much sense.
Long-term memory is slightly more complex because information stored within it is separated into different types that may be affected dependent upon which areas of the brain have been damaged:
- Emotional memory: This type of memory will be triggered by an emotional attachment to an event, place or person
- Autobiographical memory: This type of memory concerns the history of an individual’s life and all the information that they have gathered whilst they have been alive
- Procedural memory: This type of memory concerns anything that requires knowledge of how to do something or anything that needs to follow a procedure, such as making a cup of tea or putting socks on
- Semantic memory: These memories concern general knowledge and facts about the world, such as who the Prime Minister was in 1975 or what year England won the World Cup. It also helps an individual find the correct word to use in communication, so is often severely affected in those with dementia
he effects of short-term memory loss can be very distressing. Individuals may struggle to remember the content of a conversation that they have just had or they might forget that they have just eaten a meal and start to prepare another one. Additionally, it is common for someone who has short-term memory problems to repeat themselves over and over again, which can be very distressing to their family as well as a source of great frustration for them and for any care workers as well.
Since short- and long-term memories are stored in different areas of the brain, it is possible for someone who has a very poor short-term memory to be able to recall incidents that happened to them many years ago. In particular, autobiographical memories tend to stay fixed for people as they age, which is why so many older people delight in reminiscing – something which has proven to be excellent therapy for individuals with dementia.
However, if the hippocampus area of the brain is affected by dementia, then the individual will have problems recalling memories that are held in their long-term memory store. This tends to be very upsetting for family members because their loved one can no longer recall who they are because the area of the brain that is called upon to match a face to a name has been subject to disease and therefore is no longer functioning adequately.
Memory loss is one of the first and most prominent symptoms of dementia; sadly, it cannot be reversed and it will certainly get worse as the condition advances.
When someone’s ability to recall information from either short- or long-term memory deteriorates it can have a significant impact on other areas of their life and of themselves. For example, changes may be noted in the following:
- Their personality
- Their mental and physical health
- Their behaviour
- Their sociability
- Their lifestyle
- The place where they live or their general environment
Mental and physical health can also be negatively affected by memory loss. Physical health may deteriorate because an individual forgets to take their medication or forgets that they even have a condition that needs to be monitored, such as diabetes. Mental health issues such as depression become more prevalent because the individual becomes angry and frustrated that they can no longer live as independently as they used to due to dementia.
Lifestyle and sociability are affected by memory loss because often individuals may not feel like socialising. This could be because they fear judgement by others or fear that they will be embarrassed by their condition if they cannot remember someone’s name or an anecdote that has been discussed. Lifestyle changes may need to be made if someone was previously very active in something but they now find it difficult due to memory loss. Activities such as walking, needlework, photography and playing a sport can be difficult if the part of the memory which is affected means they cannot remember how to carry the activity out; for example, how to load film into a camera or how to download pictures from it.
Problems Due to Communication Issues
Dementia presents many challenges in communication and interaction for those people who have the condition. Communication is a vital part of life; without it individuals are unable to let their needs be known and this can have a very negative effect on their overall well-being.
One of the most common initial problems for someone with dementia when they are interacting with others is the inability to find the correct or suitable word to use in the context of the conversation. This happens to everyone every now and again, but with dementia it is the fact that the individual cannot even be prompted in finding the correct word.
When an individual cannot follow a conversation, this is likely to make them avoid these situations in the future, perhaps because of embarrassment or maybe because they found it too frustrating.
The inability to recall information is a common issue with people who have dementia. An individual will often repeat themselves in conversation or forget about what was being discussed in the conversation previously. The individual who has dementia will have no recollection of it at all, even though it has only been spoken about a very short time before.
Not being able to make connections also affects the conversation because this means that body language can be misinterpreted. For example, someone who can no longer read what certain gestures mean may flinch as though they are about to be attacked when someone reaches out to hold their hand.
Problems in an Individual’s Environment
Every day people carry out tasks that involve following an instruction or a sequence of events and this is most often done without any kind of conscious thought. They do not usually cause problems unless they are very complex or being carried out for the first time. However, with dementia, deterioration in the area of the brain which is responsible for following instructions means that individuals will often be unable to complete a simple task which they have been doing all of their lives.
Sometimes it is not the actual carrying out of each part of a sequence that is problematic for someone with dementia but the order in which the sequence should be carried out. Someone may know how to put something in the microwave and how to operate its timer but they cannot follow the sequence of instructions in order to cook the food properly, which can result in things being burnt or partially frozen foods being eaten.
It is very common for people with dementia to repeatedly ask for an instruction to be repeated or for them to carry out the same instruction over and over again without moving on to the next one.
One of the most distressing things for families of those people with dementia is when they are unable to recognise familiar faces. This can result in them not knowing whom they are speaking with, which can sometimes result in them being quite afraid because everyone appears to be a stranger.
Failure to recognise things does not just apply to faces, this can also be present as an inability to recognise objects and places, all of which the individuals will have encountered on multiple occasions during their life. This can result in extreme confusion when someone is offered an object, such as a pen to write something down.
Being unable to recognise a familiar place can be very frightening for an individual with dementia because they may be able to recognise a place one day and then be completely mystified as to where they are the next.
Finally, difficulty in interpreting an environment for someone with dementia is affected because of problems with general understanding of what is happening in a situation; examples of which might be:
- Problems with following what is happening on a TV programme or in a book
- Repeatedly asking the same question about the same thing over and over
- Problems with telling the time
- Being confused about what to do next, even in very familiar situations

An Individual’s Dementia and How It May Affect Others
Often with dementia, and especially in the later stages, the symptoms of the condition affect the family and friends of the individual as much as it affects them. Many family members and carers report that living with or caring for someone who has dementia can be an extremely challenging time, and for this reason it is essential that a full support network is in place both for the individual and for those around them. This means that if someone is feeling especially stressed about the situation, they know they have someone they can rely on who will simply listen to them if this is what is needed. Others who are not involved in the care of the individual may be able to provide an impartial view on the circumstances, which others may be unable to see because they are so emotionally involved in caring for the person who has dementia.
It is natural for the loved ones of the individual to feel angry at the diagnosis of dementia because the effects of the condition will be life-changing (if not at that time but certainly later). Anger may also be caused by caring responsibilities, lack of support from other family members and also possibly by the behaviour of the individual. The individual’s behaviour may also cause humiliation and embarrassment because one of the symptoms of dementia is that the individual will become less inhibited and may not respond appropriately in social situations. This may mean that they swear at people who they don’t know or that they may attempt to leave the house dressed in underwear or nightwear.
Family members often feel a sense of guilt because there is nothing that they can do to stop the progression of the condition. Some may think that they could do more to help the individual but are unable to because of their own commitments, such as their children or their job, which already take up a lot of their time. Conversely, some family members may feel overwhelmed because of the caring commitments that they have taken on and this can lead to feelings of resentfulness because they have given up their own life to care for someone else. These feelings may be made worse if the individual exhibits behaviour that challenges others. This is because it can be very difficult to deal with, particularly if the individual becomes aggressive, which can happen in the later stages of dementia due to changes in the brain. This behaviour is trying to communicate something that the individual themselves cannot.
If someone’s life has changed because of their caring commitments, this may mean that they spend less time with their partner and children; often, unpaid carers are the children of the person who has dementia. This may lead to family conflict because the person’s family feel as though they are being neglected in favour of the person who has dementia.
Family conflict can also occur when trying to help the individual to decide about their future. Many people who are diagnosed with dementia will plan ahead and make it very clear from the outset what they want to happen with their home, their finances and when they would like to have the responsibility of making decisions given to someone else. When plans are in place like this, the future can be much easier to cope with because things have already been decided. However, if plans have not been made then family members may disagree about the best course of action to be taken in order to bring about a resolution to how the individual will be best cared for.
Some individuals who have dementia report that once the condition has been diagnosed that they have reduced contact with some of their family and friends. This is likely because other people don’t know what to say to them because they are not educated enough about the condition to know what it really entails. Many will rely on negative stereotypes gained from other people and this can make their view of someone who has dementia to be very inaccurate.
Reduction in contact with family and friends leads the individual to be at risk of isolation, and this can be a precursor to other types of mental illnesses such as depression and anxiety. Additionally, someone who is providing the full-time care may also be subject to isolation because caring can be a very demanding and time consuming role meaning that they have no time for themselves, which can lead to their own health suffering.
Finally, a sense of loss is understandable for others because the person that they once knew seems to be changing and being lost as time passes. This can be very distressing for everyone involved and the sense of loss is impacted in the later stages of dementia when the death of the individual becomes inevitable.
Interventions for Dementia
An early diagnosis of dementia is essential in ensuring that individuals are given early access to all possible types of treatment. Early diagnosis also means that if one treatment does not appear to be having positive effects, this can be amended – something that may be too late if a diagnosis were not done early enough.
Treatment will initially involve a thorough assessment by a GP, who will be able to advise about risk factors and other aspects of a person’s life that may be impacted by their diagnosis. At this point, it is usual that medication might be offered to an individual. Although, of course, they do not have to accept this and many choose not to because they do not want to rely on being medicated for the rest of their lives.
Dementia worsens because of gradual but consistent damage to brain cells, but there are some types of medication that can slow the damage down in Alzheimer’s disease and DLB, which are:
- Donepezil
- Rivastigmine
- Galantamine
- Memantine (Alzheimer’s only)
This medication is not a cure for any type of dementia but it may give individuals further opportunity to remain independent for longer, lessening the possibility of them having to live in residential care for a much longer time.
For vascular dementia, it may be possible to manage the symptoms of dementia by offering the individual types of medication that promote other aspects of their health that are thought to be linked to this type of dementia. So, medication to control blood pressure and cholesterol may be a useful alternative to the medications that are meant specifically for dementia.
Treatments do not just require medication though, as individuals are using therapy more often as a way of managing their condition. Not only does this help their condition but it can give individuals a much better quality of life because it improves their overall well-being.
There are several types of therapy; these include:
- Counselling – a person-centred method where the therapist guides the individual to identify their own solutions
- Cognitive behavioural therapy (CBT) – this type of therapy helps the individual to amend the way they think and behave, often in response to some kind of trauma; in this case it will be the diagnosis of dementia. Someone who is newly diagnosed with dementia may isolate themselves and avoid going to events or continuing with old hobbies. CBT can help a person with dementia continue to live as normal a life as possible by giving them confidence to continue doing activities that make them happy. For example, someone may have regularly taken dance lessons but since their diagnosis they feel too ashamed or embarrassed to attend. Families and carers can benefit from attending sessions with the individual so that they can assist them in using the techniques when they are not in a therapy setting
- Life story and reminiscence work – this type of work is usually shared between the person with dementia and their family, friends and carers. A scrapbook or photo album is used to record details of the person’s life experiences, values and beliefs
- Complementary therapies – many individuals find massages, meditation and light therapy to be helpful in promoting overall health and well-being
Some individuals will benefit from seeing a psychiatrist (a specialist medical professional who deals with mental illnesses). They will be able to advise what has already happened to the individual and what they and their family can expect next. An occupational therapist can assist the individual to maintain their independence and can offer advice and guidance about how they can remain active, any modifications that might benefit them in their home and how carers can best work with them in order for them to retain the skills that they currently have for as long as possible.

Helping someone with dementia
If the individual is still living at home, then their family can be an invaluable source of assistance to them. Having open communication is vital so that the individual feels as though they can ask for help when they need it. Therefore, the importance of a positive and supportive relationship between the person who has dementia and their partner and other family members is essential.
The physical care needs of the individual may be attended to by others. This can include helping them to get in and out of bed, to shower and wash, go to the toilet, ensure that they are eating proper meals at appropriate times and taking any appropriate medication as well. It is sometimes found that individuals who have dementia and who are still living at home neglect aspects of their physical care, sometimes because they simply cannot remember what they need to do or how they need to do something. Family members may find a rota system to be useful so that everyone knows who is helping, what they are helping with and when. For example, someone’s daughter may always come and help in the morning on her way to work, she helps the individual to get out of bed and to prepare their breakfast. Not only does this provide the reassurance that the individual is being monitored but it can help build family relationships as well because everyone is playing a part in the care of their loved one.
If possible, it may be useful for some modifications to be made around the home of the individual to help them feel safer. This can include handrails around the home so that they have physical support and possibly changing a bath for a shower (a shower would be much easier to get in and out of and lessens the risks of scalding or even drowning). Clothes that are simple to put on and take off can also help the individual to retain their independence.
The psychological and emotional needs of the individual should not be ignored. A diagnosis of dementia can be a very frightening and lonely time, so it is essential that the individual is comforted and shown love, affection and companionship by the people around them. This is not always easy because family members will also be affected by the diagnosis as they will likely know the eventual effects and changes that will occur to their loved one because of it. Often though, people don’t know how to react to a diagnosis of dementia because they don’t know enough about it. Therefore, reading up about what it is and how it can be managed can be very useful in bringing about empathy and compassion from the people around the individual.
It is also essential that the individual is enabled to keep their identity and is in touch with their history as much as possible. This has been shown to improve the quality of life for those who have dementia, and ‘reminiscence therapy’ is something that is carried out with individuals to help them retain memories of their past and remember who they are. Family members can get great enjoyment from putting together a life history book full of pictures and short anecdotes so that the individual can refer back to it and remind themselves of their past and of who important people are. A life history book is also very useful if the person has to go and live in residential accommodation because it helps staff to know something about them and therefore how to tailor their care to meet the unique needs of the individual.
In the later stages of dementia, it is likely that the individual’s ability to make decisions for themselves will be in decline. Therefore, giving them support with their finances and decision making will ensure that they are given every opportunity to retain their independence. Knowing what the individual’s wishes for the future are will help to ensure that they are carried out in the way that they have requested. For example, some individuals will request that if they have to go into residential care that their savings are used to pay for the care and that their house is sold with the profits going to their children. They may have decided that they want to go into care only when they can no longer attend to their personal hygiene or when they become too difficult for their partner or other family members to cope with alone.
The Mental Capacity Act 2005 helps to protect individuals who cannot make decisions for themselves by ensuring that any decisions made are done in their best interests. Knowing what the individual’s rights are can also help to guide carers through what can be a very difficult time both emotionally and legally because some legislation is very difficult to navigate.
Whatever stage the individual’s dementia is at, simply being there to help and support them in any way possible will help to ensure that their quality of life is not inhibited too much by their condition. Many individuals who have dementia state that it is the fear of becoming a burden to their family that is the most frightening part of dementia. Ensuring that they do not feel this way will give them hope and reassurance and their happiness and overall well-being may remain positive as a consequence.
The Local Resources and Treatments for dementia
The local resources and treatments available to someone who has dementia would depend on what their individual needs are and how far their condition has progressed.
In the early stages of dementia, individuals and their carers may benefit from knowing more about the condition and what some of their options are with regards to treatment, management and possibly even with accommodation once the illness progresses. There are several charities and organisations who can assist with these issues:
- The Alzheimer’s Society
- Mental Health Foundation
- Age Concern
- The Anchor Trust
The Alzheimer’s Society and Mental Health Foundation aim to improve the lives of people who are living with a mental illness. They offer free advice and services that will help inform individuals and their carers about specific mental illnesses and how their lives can be improved despite their diagnosis. They also arrange charity events, which can be a very enjoyable activity for individuals to get involved in. Knowing that they are making a difference and raising awareness of the condition can be very positive for someone’s self-esteem and therefore their overall well-being.
Age Concern is a charity that works specifically with older people. They offer advice on a huge amount of issues that may be relevant to the person who is living with dementia and their family and carers. Everything they do is tailored to meet the needs of older people and they employ people who are professionally trained in many areas to offer support and advice about issues such as:
- Money
- Health and well-being
- Living arrangements
- Work
- Travel
- Lifestyle
Their work helps to ensure that people are not forgotten simply because they are older and this is even more important for people who have dementia as this is an attitude they will also face as well.
The Anchor Trust helps to provide housing and care for older people. They will assess the current living conditions of an individual with dementia and then offer advice about whether any modifications could be made or if they would benefit from living elsewhere. They have a range of professionals working with them to ensure that their services are accessible to all.
Other types of local resources include:
- Care homes
- Hospitals
- Domiciliary care
- Respite care
- Supported housing
Where an individual with dementia lives is very important because they will need to feel secure, comfortable and settled in an environment that is not going to aggravate their condition further.
A care home may be needed if the individual and their unpaid carers can no longer manage their needs. This type of accommodation can provide around-the-clock care and they have professionals on site to help with any specific needs. A care home may be something that an individual is resistant to at first because it may cause them confusion and upset. However, often in the later stages of dementia, this may unfortunately be the only option to manage the care needs that the individual has.
Hospitals will help individuals who have become ill or injured because of their condition but it is unlikely that they will be a long-term option for someone. Due to their condition, some individuals will need to be hospitalised once they have had a diagnosis of dementia, possibly because they have fallen and injured themselves or they have been more ill than they would normally be due to an infection. Hospitals can care for an individual until a suitable alternative place of accommodation has been found.
Domiciliary care is for those individuals who are maintaining their independence by remaining at home. Care workers will attend the individual’s home, often several times a day, to ensure that they are taking adequate care of themselves. This may mean that they help with some personal hygiene tasks, prepare meals and help with medication. The care workers will also be able to monitor the individual for any changes in their condition, which means that the care and support that they receive needs to be amended.
Respite care enables carers to take a break from their caring role because the individual with dementia will be given short-term accommodation by the local authority. Respite care is useful for carers because it gives them a chance to have time for themselves, which may only involve them catching up on much needed sleep. Caring can be a very demanding role and it is advised that carers take up offers of respite care or request it when they need to so that their own health is not compromised by their caring duties.
Sheltered accommodation enables the individual to retain some of their independence whilst also being monitored by someone as well. The accommodation will be smaller and easier to manage, often with adaptations to make things easier for the individual who lives there. There will often be communal areas where residents can get together and many offer social events for residents to become involved. This can be very useful in preventing isolation and many individuals with dementia will enjoy remaining socially active for as long as they are able.
Many sheltered accommodation locations will have a warden who lives on site who can provide assistance immediately if it is needed. However, some will not provide this but will provide a 24-hour emergency help system through an alarm instead.
Factors that can negatively affect someone with Dementia
When someone has been diagnosed with dementia, it can be a very difficult experience and the individual may find that they are much more sensitive to what is said to them; even if the words are meant encouragingly or are not meant to offend.
Ill-considered words or actions may lead the person with dementia to exhibit agitated or aggressive behaviour because, often, this is the only way that they can communicate the fact that they have been hurt by what someone has said or done. One of the symptoms of dementia in the middle and later stages of the condition is an inability to communicate effectively because the individual cannot find the words to express what they want to say. Therefore, rather than them being able to tell someone that they have been hurt by their words, they have to resort to behaviours that challenge others to try and make themselves understood.
Agitation for someone with dementia can lead them to repetitive behaviours. This may mean that they repeatedly carry out an action such as tugging at a piece of clothing or rocking in their chair. It may also mean that they ask the same questions over and over again or repeat the same information in the same way. This can be very challenging for the people who provide care and support but can also be avoided by others knowing how their words and actions may provoke such negative consequences.
Individuals who are spoken to in a kindly and considerate manner are far more likely to be relaxed and confident because they have the reassurance that they are not being judged or ridiculed by others. Even though this might not actually be happening, many individuals may well perceive that people are treating them negatively, so it is important to give them reassurance that this is not the case. Individuals who are confident are more likely to be busy and involved in their lives and are therefore less likely to be at risk of isolation.
Knowing about the individual and their life history can lessen the chances of the individual exhibiting behaviour that challenges others because the behaviour may be able to be interpreted as communicating a need or something that is very important to them. For example, if someone were to wander around at 3pm every day, this might simply be misinterpreted as a sign of their dementia and they might be told to sit down because their behaviour is upsetting others. However, it may transpire that at this time, the individual left the house every day to collect their grandchild from school. Knowing about this can lessen the behaviour because the individual could be distracted or could even go on a short walk each day at that time so that they feel as though they have done what they need to do.
Finally, it is vital that person-centred care approaches are always applied with anyone who needs care and support. This means that the individual is put at the centre of their care and takes an active part in how it is planned and carried out. By leaving the individual out of important decisions about their life shows complete disrespect for them as a human being and this can also result in challenging behaviour. Someone who is actively involved in their care will feel as though their dignity has been maintained and that they are making an active contribution to society and therefore retaining their independence for as long as possible.



